Happiness Is A Skill was created as an outlet for me to reach the kind of people who email me every day. Ever since my Washington Post Article, “I spent half my life on antidepressants. Today, I’m off the medication and feel all right” became the #1 read piece on WaPo National the day it was published, my inbox likes to fill up with people who are struggling to get off their antidepressants or benzodiazepines. I respond to every person who contacts me, and often that correspondence leads to a longer conversation.
About 12 weeks ago, after one of these conversations melted two hours away from my day, it occurred to me that I was spending a lot of time saying similar things to lots of different people. Why not take all that information and distill it down into a digest that could reach lots of people at once? And so Happiness Is A Skill was born. There are two overarching themes of these emails. First, people are desperate to find relief from the pain of withdrawal, all while trying to process the anger they have for prescribed drugs and doctors that were supposed to help them. Second, they are looking for someone, anyone, who understands. Psychiatric drug withdrawal is an excruciatingly long and lonely process that you simply cannot relate to unless you have experienced it. It’s rare to encounter another person going through withdrawal in the wild because people in severe withdrawal probably aren’t leaving their house. (And those who are experiencing mild or moderate withdrawal are likely so irritable that they aren’t exactly projecting warm fuzzies.)
Until recently, antidepressant withdrawal was swept under the rug by psychiatrists and doctors, largely due to a lack of substantial research surrounding long-term use and tapering. (Antidepressants and benzos are designed, studied, and tested for short term use, i.e., weeks. There is not a single study on the effects of long-term antidepressant use, and yet 1 in 4 people on antidepressants have been taking them for more than 10 years.)
But in 2019, a group of American and British psychiatrists came together and urged national withdrawal guidelines to be updated after they “discovered” what many patients already knew: it is a hell of a lot easier to start taking antidepressants than it is to get off of them. In a systematic review of existing research, the authors determined that “nearly half of those experiencing withdrawal (46%) report it as severe, and that reports of symptoms lasting several months are common in many recent studies.”
The authors go on to say that their evidence directly contradicts the position of the UK’s National Institute for Health and Care Excellence (NICE) guidelines, which state that “[withdrawal] symptoms are usually mild and self-limiting over about 1 week.” In short, this research shows that half of all antidepressant users will likely experience withdrawal of a substantially longer duration and severity than current guidelines recognize. Shockingly (to this American, anyway), the NICE guidelines were updated to reflect these findings, giving suffering withdrawal patients a smidgeon of validation. All this to say that the tides are changing. My article and others like it are finding space in mainstream media and a new cohort of psychiatrists and researchers are starting to take our claims seriously. But arguably the biggest contribution to bringing this issue to light is the new documentary, Medicating Normal. I had the pleasure of watching a screening a few days ago, and it both broke my heart and fed the fire within me.
A synopsis:
“Combining cinema verité and investigative journalism, Medicating Normal follows the journeys of a newly married couple, a female combat veteran, a waitress and a teenager whose doctors prescribed psychiatric drugs for stress, mild depression, sleeplessness, focus and trauma. Our subjects struggle with serious physical and mental side effects as well as neurological damage which resulted from taking the drugs as prescribed and also from attempting to withdraw. Says one psychiatrist, ’There’s not a chemical on the planet, to my knowledge, that can require years to taper — not Oxycontin, not crack cocaine, not heroin, and not alcohol. But psychiatric medications, any tapered patient will tell you, can take sometimes years if possible, at all.’ … [Medicating Normal] is the untold story of what happens when profit-driven medicine intersects with human beings in distress.”
Statistically, a good chunk of Happiness Is A Skill readers are taking some form of antidepressant or anti-anxiety/benzodiazepines like Xanex or Ativan. For those people, none of this is meant to scare you or bully you into getting off the drugs. You do you. However, if you ever do want to get off these drugs, I implore you to do your research and work with your doctor to create a slow, deliberate tapering plan. Doctors are not required to give patients informed consent when it comes to psychiatric drugs, nor are they well versed in safe withdrawal. It’s not their fault. The medical system simply doesn’t teach them how to take people off these medications. It is possible to wean off psychiatric drugs safely and with few side effects, but the techniques for doing so are being developed at a grassroots level by people who have experienced it, like me. For more information on safe withdrawal, check out SurvivingAntidepressants.org, Mad In America, and the Inner Compass Initiative. You can also email me directly. Lastly, Medicating Normal is being screened virtually at several film festivals and hosted events. I would recommend it to anyone who is taking antidepressants or benzos, but I believe it should be required watching for all practicing psychiatrists and doctors. You can find tickets and upcoming screenings here.
Coming September 6, 2022
May Cause Side Effects
Brooke’s memoir is now available for preorder wherever books are sold.
This is a heart-rending and tender memoir that will start conversations we urgently need to have. It’s moving and important.
Johann Hari, author of New York Times bestseller Chasing the Scream and international bestseller Lost Connections: Uncovering the Real Causes of Depression—and the Unexpected Solutions
More articles from the blog
see all articles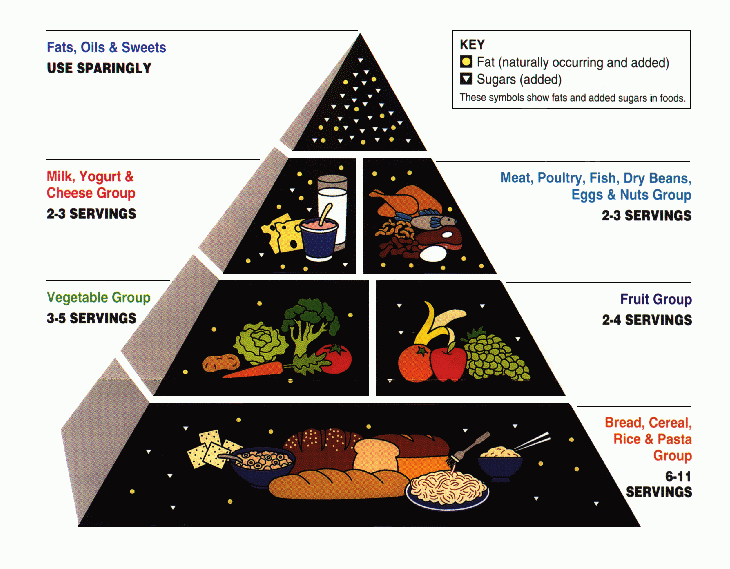
July 9, 2025
How World War II, cigarette companies, and an obscure 1937 law determine what you put in your mouth today: A Short History of the Sad, Modern American Diet.
read the article
July 2, 2025
“What do all fat, sick, unhealthy people have in common? At least this: they all eat.: An introduction to a new series about diet, psychiatric drug withdrawal, and performance.
read the article
June 25, 2025
Bad Medicine, Antidepressant Withdrawal, and the Incalculable Costs of Medicating Normal: My full talk at the University of Nevada, Reno Medical School
read the article
June 18, 2025
