September 2, 2022 • Brooke Siem
The Ashton Manual: A guideline for withdrawing from psychiatric drugs
As one of the few people to have successfully published an article about the realities of antidepressant withdrawal in a major newspaper, my inbox is filled with inquiries from people whose experience is similar to mine. One of the most common comments is from people who say their doctors pulled them off psychiatric drugs over the course of days or weeks, leading to unbearable withdrawal symptoms.
This type of message makes me irate because as far as I’m concerned, this is patient abuse. Dangerous psychiatric drug withdrawal is avoidable, and when it does occur under a doctor’s care, it is a direct result of physicians not doing their due diligence on research that has existed for over twenty years.
A little background:
Despite years of patient suffering, research into antidepressant withdrawal has been a low priority for doctors and psychiatrists. The first systematic review of antidepressant withdrawal did not even exist until 2015, a full twenty-eight years after Prozac was first released to the public in 1987.
Finally, in 2019, the first comprehensive systematic analysis of antidepressant withdrawal found that more than half of people coming off antidepressants experience withdrawal symptoms, and half of those—like me—experience severe withdrawal (Davies & Read, 2019), also known as protracted acute withdrawal syndrome (PAWS). A separate, 2020 study of those suffering from antidepressant-associated PAWS found that participants experienced withdrawal symptoms for an average of thirty-seven months, with eighty-one percent of participants reporting suicidality as a direct effect of their withdrawal symptoms. (Hengartner, Schulthess, Sorensen, et al., 2020).
The research on withdrawing from benzodiazepines (Xanax, Valium, Klonopin, etc.) is much more robust. Benzodiazepines and antidepressants both emerged in the 1950s, but it was benzodiazepines that became known as “mother’s little helper” and were prescribed to keep housewives from becoming “hysterical women.” Their immediate, tranquilizing benefit thrust them into the spotlight, and as the decades went on, their reach became more ubiquitous, eventually leading to the benzodiazepine addiction crisis.
Enter Dr. Heather Ashton, a British psychopharmacologist and physician with a focus on benzodiazepines dependence and withdrawal. It was Ashton who first realized that long-term use of benzodiazepines led to physical dependence, but that short-term use sometimes had its benefits. (Remember the Thai soccer team stuck in a cave back in 2018? They were rescued in part thanks to Xanax, which was part of a cocktail used to lower their anxiety before they were sedated and guided out of the cave. A perfect, one-time use of the powerful drug.)
Ashton dedicated her life to working with people addicted to the benzodiazepines. In 1999, at 70 years old, she published “Benzodiazepines: How They Work And How To Withdraw,” now known as The Ashton Manual.

The Ashton Manual advocates for extremely slow tapers, much slower than the average recommendation by physicians (and most governments.) Faster tapers can lead to restlessness, irritability, insomnia, muscle tension, racing heartbeats and other debilitating symptoms, much of which can be confused with anxiety which leads the patient to pop another pill to alleviate the symptoms.
If you’re a long time reader of Happiness Is A Skill and/or have read some of my other work, you might think benzo withdrawal sounds similar to antidepressant withdrawal, and you would be correct. Although The Ashton Manual initially focused only on benzodiazepines, the sharp rise in antidepressant use in the 2000s led Ashton to update her guide to include antidepressant withdrawal. Today, the distinction between withdrawing from antidepressant or benzodiazepines is minimal. Both should be done extremely slowly and done under the care of an informed physician.
The Ashton Manual is available for free on Benzo.org.uk or via Kindle. It is an invaluable resource for anyone struggling to get off psychiatric drugs or for physicians looking to understand how to manage a patient’s taper.
Lastly, if you feel your health is being mismanaged or you are getting resistance from your doctor about taking a slow and controlled taper, do not be afraid to seek out a different qualified professional. I cannot over stress how not all MDs are created equal, and that there is someone in your area who understands the delicate nature of psychiatric drug withdrawal who will help you create a plan.
More articles from the blog
see all articles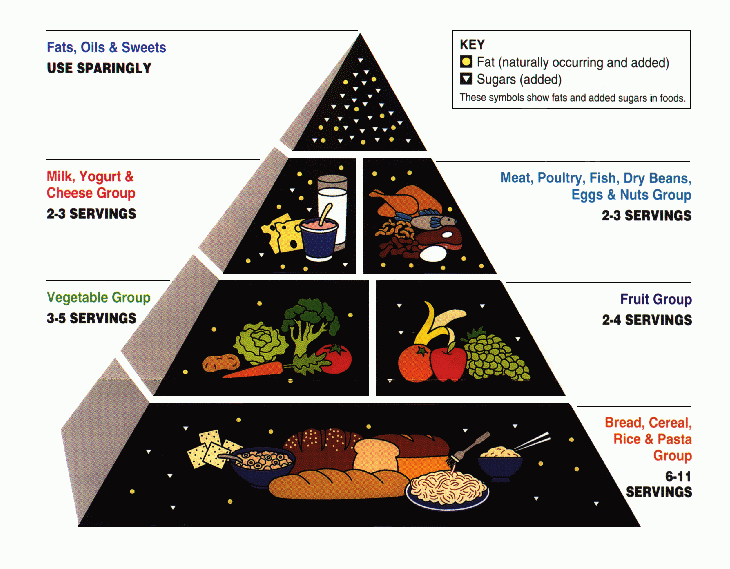
July 9, 2025
How World War II, cigarette companies, and an obscure 1937 law determine what you put in your mouth today: A Short History of the Sad, Modern American Diet.
read the article
July 2, 2025
“What do all fat, sick, unhealthy people have in common? At least this: they all eat.: An introduction to a new series about diet, psychiatric drug withdrawal, and performance.
read the article
June 25, 2025
Bad Medicine, Antidepressant Withdrawal, and the Incalculable Costs of Medicating Normal: My full talk at the University of Nevada, Reno Medical School
read the article
June 18, 2025

